Types of Wounds Managed
Debridement
Removal of nonviable (dead or infected) tissue to promote faster wound healing and significantly reduce the risk of infection. This process helps create a clean wound bed, allowing healthy tissue to grow more effectively. Different methods of debridement may be used depending on the wound type, including surgical, enzymatic, autolytic, or mechanical techniques, all tailored to the patient’s condition.
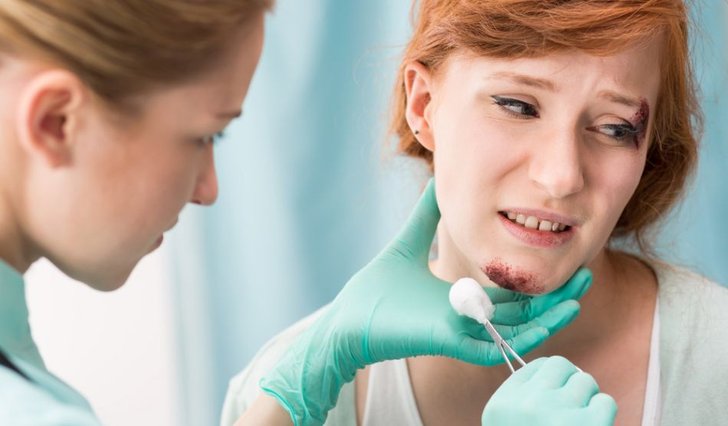
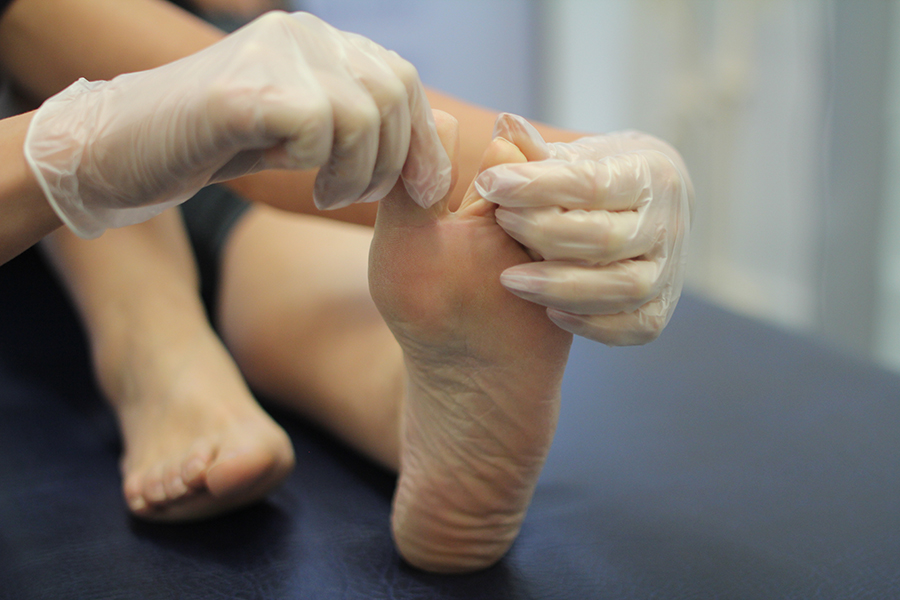
Infection Prevention & Management
Early identification and proper treatment of wound infections to minimize complications and avoid delays in healing. This includes regular wound assessment, use of appropriate antimicrobial dressings, and, when necessary, antibiotic therapy. Maintaining a clean environment and proper hygiene practices plays a crucial role in preventing infection and ensuring optimal recovery outcomes.
Negative Pressure Wound Therapy
An advanced wound care technique that uses controlled suction to remove excess fluid, reduce swelling, and promote the formation of healthy new tissue. This therapy improves blood flow to the area, decreases bacterial load, and accelerates healing, especially in chronic or complex wounds.
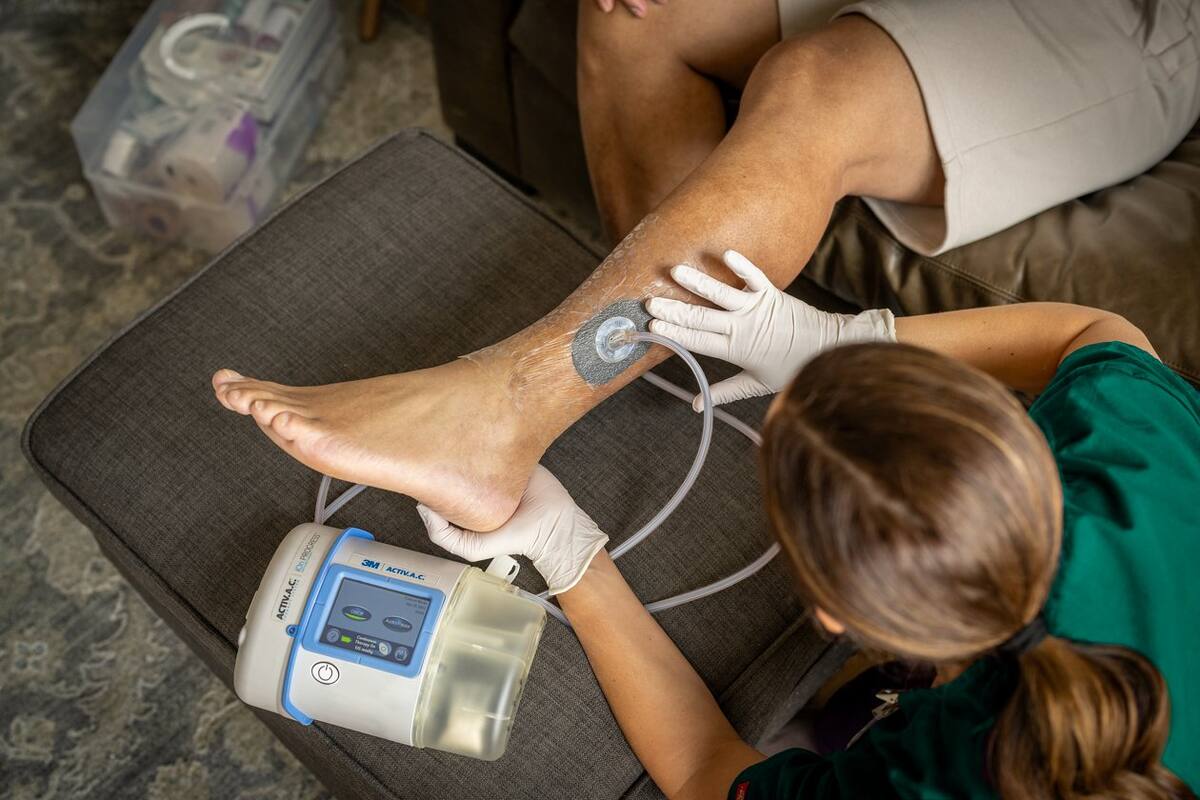
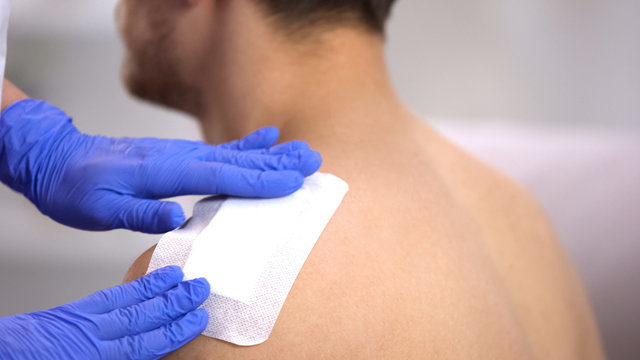
Specialty Wound Dressings
Application of advanced wound care products, including hydrocolloids, alginates, foam dressings, and bioengineered skin substitutes when clinically indicated. These dressings are selected based on the wound type, moisture level, and stage of healing to create an optimal environment for recovery while protecting the wound from external contaminants.
Coordination of Care
Close collaboration with physicians, home health agencies, and facility staff to ensure a comprehensive and consistent treatment plan. This team-based approach improves communication, enhances patient outcomes, and ensures that every aspect of the patient’s wound care journey is properly managed and monitored.


Patient & Caregiver Education
Providing clear and practical guidance on wound care management, including proper dressing techniques, nutrition for healing, skin protection, and pressure offloading strategies. Educating patients and caregivers empowers them to actively participate in the healing process, reduces the risk of complications, and supports long-term recovery and prevention of future wounds.
